Editor’s Note
This excerpt from a review on digital dentistry outlines foundational principles for implant-supported prosthetics in edentulous jaws, comparing fixed and removable options while noting established survival rates for fixed restorations.
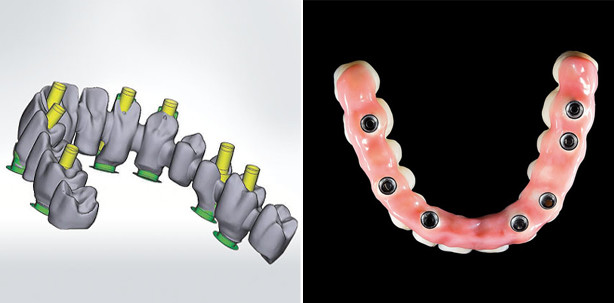
The restoration of the edentulous jaw is a classic indication for implant-supported prosthetics (Zitzmann and Marinello 2002). In principle, both a fixed, purely implant-supported restoration on six to eight implants and a removable restoration with a reduced number of implants are possible.
Fixed, implant-supported prosthetic restorations show high survival rates for both implants and superstructures (Jung et al. 2012, Pjetursson et al. 2012). However, the evaluation of studies also showed that implant-supported crowns and bridges have an increased incidence of technical complications. Primarily, loosening of abutment or retention screws of the superstructure, loss of retention in cemented restorations, and fractures of the veneering ceramic are to be expected (Jung et al. 2012, Pjetursson et al. 2012). In particular, large-span, implant-supported bridges, as used in the restoration of the edentulous jaw, show increased complication rates. Papspyridakos et al. (2012) demonstrated in a systematic literature review for implant-supported bridge constructions in the edentulous jaw that after a ten-year observation period, only 8% of the constructions were free of complications. There was a high incidence of peri-implantitis (40%), screw fractures (20%), and veneering material fractures (66%). It can be concluded that with increasing size of implant-supported bridges, higher complication rates are to be expected. The comparatively high technical complication rate becomes particularly significant with large, cemented, and ceramic-veneered, implant-supported bridges (Fig. 1). In the case of such a complication, repair of the veneering is possible if the restoration can be removed non-destructively. However, it is associated with high dental laboratory effort and corresponding costs. The repair usually takes several working days and therefore requires renewed provisional restoration of the patient. Furthermore, it must be considered that cemented, jaw-encompassing bridge constructions are difficult to access for home oral hygiene (Fig. 2). This is also reflected in the results of the already cited review in an increased rate of gingival hyperplasia and a corresponding peri-implantitis rate. Moreover, with cemented, multi-unit bridges, it must be assumed that excess cement is difficult to remove. Clinical studies have repeatedly shown that excess cement can be a frequent cause of peri-implant inflammation (Korsch et al. 2013, Linkevicius et al. 2012, Sailer et al. 2012, Vindasiute et al. 2013). The use of screw-retained bridges therefore offers the advantage, due to their conditional removability, that they can be easily removed in case of repairs. Additionally, the implants are more accessible during professional hygiene measures as part of maintenance therapy. Avoiding cementation of the construction also reduces the risk of iatrogenic peri-implantitis.
Fig. 1: Ceramic fracture on an externally fabricated and cemented, multi-unit bridge after eight months of wear.
Fig. 2: Increased deposits on a provisionally cemented, multi-unit, implant-supported bridge after twelve months of wear.
Fig. 3: Initial finding with severely periodontally compromised remaining dentition.
Fig. 4: Situation after insertion of implants in the upper and lower jaw.
Fig. 5: Intraoral splinting of impression posts with a light-curing composite for improved fixation in the impression material.
Fig. 6: Impression of the implants using the pick-up technique with a high-strength polyether impression material.
Fig. 7: Fabrication of a working model with a removable, flexible gingival mask.
Fig. 8: Selection of suitable abutments for later central screw retention (ANKYLOS Balance Base).
Fig. 9: Virtual construction of the bridge framework with conventional central screw retention. The vestibular position of the screw access openings leads to aesthetic impairments. (Partial screenshot of software screen)
Fig. 10: Modified design with the specific angulation of screw channels up to 20° for the cara I-Bridge system. In this way, all access openings could be relocated to aesthetically non-critical areas.
Fig. 11: Overview of the design proposal for the bridge construction sent via email.
Fig. 12: Detailed view of the bridge framework milled from a CoCr alloy.
Fig. 13: Try-in of the milled bridge framework to check for passive fit and correct occlusal position.
Fig. 14: Basal view of the finished veneered bridge framework. The superstructure was veneered using the silicone key from the existing tooth setup.
Fig. 15: Completed, screw-retained implant bridge.
Fig. 16: Completed, screw-retained implant bridge in frontal view.
Fig. 17: Satisfied patient.
